Dermogynaecology refers to the study of disorders either dermatological, infective or functional which affect the lower genital tract and impact on the physical and psychological well-being of the patient. These conditions which affect the vulva or vagina may initially present to the family doctor, gynaecologist or dermatologist. Often a definitive diagnosis cannot be established within a particular speciality and a multidisciplinary approach is required particularly in those patients who have had a protracted clinical course complicated by intervening pathologies.
The Dermogynaecology Clinic was initially established in 1990 at the Mercy Hospital for Women under the direction of Dr Graeme Dennerstein and over a 10 year period over 2000 patients were treated until its closure in July 2000. It utilized the expertise of gynaecologists interested in diseases of the lower genital tract, in consultation with a dermatologist and a pathologist with a special interest in dermatopathology. The clinic currently operates from the private rooms of Dr Sam Sfameni at 253 Pascoe Vale Road, Essendon.
Symptoms related to lower genital tract disease may be of acute onset at the initial presentation but subsequently become chronic and long standing over many years, especially when the appropriate diagnosis and treatment has not been established. The most common vulval symptoms are pruritus vulvae (vulval itch) which is the presenting complaint in over 50% of patients, in addition to dyspareunia (painful intercourse) and vaginal discharge. Symptomatology in the vulval region may be indicative of a pathological or functional disorder requiring the appropriate diagnosis and treatment.
The most common condition encountered is that of vaginal candidiasis which repeatedly proved to be the most troublesome disorder to manage, not only for the general practitioner but also for the gynaecologist. It is essential that swabs are taken to confirm this diagnosis at all times and treatment should only be given on the basis of a positive result. Antifungal therapy (Canestan) in the form of pessaries should be inserted high in the vagina for 6 nights to clear the infection. Effectively treated vaginal candidiasis should not recur again for at least 6 months unless there are predisposing factors such as diabetes mellitus, broad spectrum antibiotic treatment, the oral contraceptive pill or pregnancy.
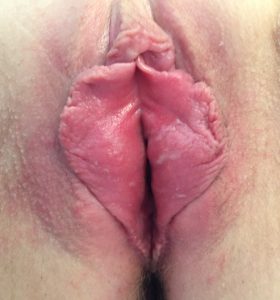
Contact irritant dermatitis occurs with almost equal frequency to and often coexists with vaginal candidiasis. Symptoms include vulvar pruritus and vulvar burning which is often the result of chemical applications to the vulvar skin, either with excessive and inappropriate hygiene practices or with attempts at self- treatment without an accurate diagnosis having been established. The diagnosis can be made on the basis of a typical history and examination of the vulva. Treatment consists of avoidance of all chemical irritants to the vulvar skin with response usually requiring at least 6 weeks before any observable improvement is noted.
Contact dermatitis of the vulva.
Lichen simplex chronicus was a frequently encountered disorder. This is often the end result of chronic physical trauma inflicted by scratching which produces lichenification (thickening) of the skin and also associated changes within the dermis marked by an inflammatory infiltrate. Skin affected by these changes becomes sore and itchy, the patient attempting to obtain relief by scratching, thus establishing a chronic ‘itch scratch cycle’. This can be very distressing for the patient and often causes other secondary pathologies to occur. A search for predisposing and aggravating factors such as stress is most important for the proper management of this disorder.
Lichen sclerosus was one of the most common skin conditions to affect the vulva. The aetiology of this disorder is unknown although there may be an underlying autoimmune basis and it is seen in all age groups including young women and children. Lichen sclerosus affects the skin of the vulva and perianal area to cause the most common symptom of pruritus. In children, scratching of the vulvar skin may cause blistering, fissuring and pain with resulting dysuria, urinary retention or constipation. In adults, long standing lichen sclerosus can cause introital stenosis and vulvar soreness resulting in dyspareunia. Vaginal candidiasis may also complicate this condition and aggravate the pruritus. In postmenopausal women, oestrogen deficiency causing atrophy of the vulva should be corrected as it may confuse the clinical picture and lead to inappropriate treatment. Lichen sclerosus with associated long standing pruritus may produce secondary hyperkeratosis and thickening (lichen simplex) of the vulvar skin giving it a white appearance. Biopsy of the vulva will confirm the diagnosis by finding the characteristic histological changes.
Lichen sclerosus is a chronic disorder which requires long term management. It is important to give the patient an explanation of the nature of the condition and the treatment available. It is important to recognize and prevent exacerbations and finally to stress the importance of follow up in order to detect any sinister lesion that may develop on the vulva.
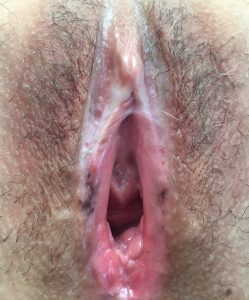
Treatment of lichen sclerosus is with topical corticosteroids which will provide relief from distressing pruritus and vulvar pain. Exacerbation of symptoms may be caused by superimposed candidiasis or contact irritant dermatitis. There is no place for the use of local testosterone cream. Surgical management of lichen sclerosus is limited to obtaining biopsies to establish the diagnosis and rarely wide local excision of any suspicious area on the vulva. Although lichen sclerosus is not thought to be a pre-malignant condition, ongoing irritation and trauma to the vulvar skin may predispose to tumour formation and hence long term follow up of patients is advised including vulvar self-examination to detect any changes in appearance of the vulvar skin.
Long standing vulvar lichen sclerosus.
Lichen planus is another skin disorder that can affect the lower genital tract and usually presents in an atypical manner when compared to other sites of the body. This again is an immunological disorder which damages components of the skin to produce on the lower genital tract an erosive clinical picture. On the vulva it is the cause of pruritus, pain and painful intercourse. The vulvar skin may have a ‘glazed’ appearance when affected and the involved area is tender to touch. The changes are less obvious in the vagina but symptoms here are often related to a chronic vaginal discharge which may stain the underwear and require the use of a pad. Diagnosis is established by taking a biopsy from the affected area which should be assessed by a pathologist with an interest in skin disorders.
Desquamative inflammatory vaginitis is a disorder that affects the lower genital tract and is responsible for a variety of symptoms which include vulvar pain & pruritus, dyspareunia and vaginal discharge. The diagnosis is difficult to establish and appropriate treatment of the vulvar skin and associated infective complications is very important in the management of this disorder.